Engineered Human Therapies
Decoding the immune system: Cogen ImmuneMedicines’ CEO Jose-Carlos Gutiérrez on changing the paradigm of antigen-based therapies
In an age where we take pills for nearly everything -- from minor headaches to life-threatening infections -- it can be hard to believe that within our bodies lie the “cures” for the maladies that afflict us. When our first line of defense against infection and disease -- our immune system -- fails us, we pay the price -- sometimes with our very lives. In our approach to treatment, we’ve often left the immune system out of the picture. It has already failed us, so we put it on the back burner and bring in the “big guns” that’ll get the job done -- antibiotics, chemotherapy, radiation.Such therapies have saved countless lives, to be sure -- but not without leaving a path of destruction in their wake, from destroyed gut microbiomes to obliterated immune systems rendering even the common cold deadly. Researchers and clinicians around the world have been working toward a new era in health care that leverages the immune system rather than ignoring it -- or even worse, rendering it all but useless.Our immune system is powerful. It is incredibly specific -- your body is full of unique immune cells primed to kill “sick” cells, such as cancerous ones. It also has a memory, and recognize incoming viruses that you were last exposed to a decade ago. These powerful characteristics are the basis for antigen-based therapies, which have shown promise for treating a variety of conditions from diabetes to cancer -- without the collateral damage associated with more traditional forms of treatment.
Decoding the key for antigen-based therapies
Immune cell specificity -- the characteristic that makes antigen-based therapies so promising -- is also a significant challenge. Sick cells display proteins on their surface called antigens; immune cells called T cells recognize antigens with unique receptors (TCRs). With one receptor for one antigen, the diversity of antigen-TCR pairings numbers in the million. Jose-Carlos Gutiérrez, CEO of Cambridge-based Cogen ImmuneMedicines (founded by Flagship Pioneering in 2017), likens these pairings to a code. With billions of unique pairs -- we are exposed to millions of viruses and mutated human cells each and every day -- decoding all possible combinations is not an easy job. But it’s one that Cogen ImmuneMedicines has taken on in a bid to propel antigen-based therapies to the forefront of medicine.Traditional antigen-based therapies rely on the creation of peptide-MHC tetramers -- a combination of the antigen of interest plus the major histocompatibility complex (MHC) molecules necessary for T cells to recognize foreign cells. The tetramers are a powerful tool to identify antigen-specific T cells. But the process of creating them is long and arduous: not only must the complexes be expressed in bacteria and then isolated and refolded, but only one complex can be made at a time this way.Cogen ImmuneMedicines’ Cogen Engine -- a platform combining multiple technologies -- utilizes high throughput, cell-free techniques to produce antigen-MHC tetramers. All components for the tetramers are encoded on a single chain of cDNA contained inside a microdroplet, where the proteins are expressed and folded. Microfluidics enables the production of thousands of barcoded complexes simultaneously, yielding antigen-MHC libraries with unprecedented diversity.
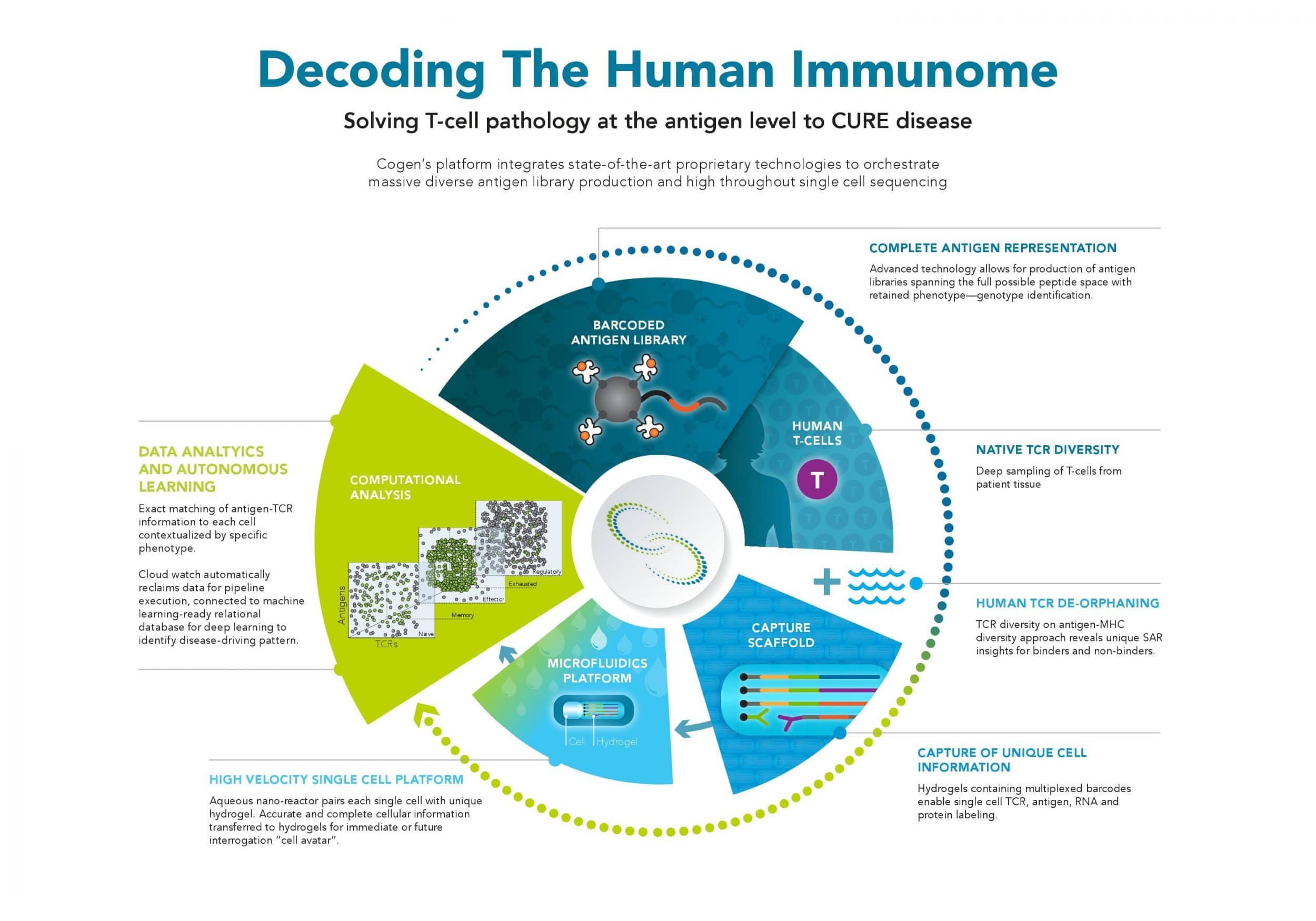
Image source: Cogen ImmuneMedicineBut the key is cracking the third part of the code: function. The antigen-MHC libraries are used to interrogate T cells in a tumor, a lymph node, or the blood, where they identify not only high-affinity antigen-TCR pairs, but also the functional state of the T cell -- effector cell, activated cell, or memory cell. Critically, this process can be done rather quickly across multiple cells within a single tumor, as well as across multiple individuals, identifying key antigen-TCR pairs associated with specific types of cancer. And unlike current neoantigen sequencing or elution-based approaches, the Cogen Engine produces a full map of all of the antigen-TCR pairs present in a tumor.“These three pieces of code, T cell receptor code, antigen code, and functional code, cell by cell, enable unique insight into the immune system,” says Gutiérrez. “And if we figure out ... the specific codes for an antigen and T cell receptor for a given disease, and give them as a medicine, we will be able to recapitulate how the immune system cures disease. The immune medicine of the 21st century is antigen and clonotype specific, very selective and very specific.”The ultimate goal is, of course, to translate the antigen-TCR code to drugs that can be used to treat cancer and, eventually, other conditions. It may seem pie in the sky -- we haven’t found cures to cancer or autoimmune conditions yet despite decades of trying -- but according to Gutiérrez the issue is not in whether a cure exists; it’s in leveraging the cures that are already inside our own bodies.“Our immune system cures us very day, using multiple antigens and multiple clonotypes of T cells doing a coordinated job, and that's what we're going to do. We're not making anything new, are already there, and our job is to reveal them. Cures are something we should aspire to,” he says.
Leading an ecosystem to leverage the power of precision immune medicine
While Cogen ImmuneMedicines strives to be a leader in antigen-TCR-based therapies, Gutiérrez stresses the power of a healthy, collaborative ecosystem. While focusing on developing robust technology to decode the antigen-TCR-function codes associated with disease, the Cogen team has formed partnerships with academic medical centers and physician scientists who will eventually use the Cogen Engine in longitudinal clinical trials to power drug development.Cogen ImmuneMedicines also offers a residency program for professors to join the team for one day a week to learn about their technology, see it in action, and share their insights. Gutiérrez says that people are increasingly recognizing the need to join what he calls a “collaborative project to discover the medicines that are already inside us.”“Eventually immune medicine will the doors to ... many other diseases. Cogen wants to lead the way, but it will be a collaborative effort, one that not only Cogen but many others in academia and industry,” he says.And, the most critical part of the collaboration is the one we’ve had with us all along -- the immune system. We now have the tools to start unlocking its full potential -- it’s time to bring the immune system back to the forefront of medicine.Join us October 1-3 in San Francisco to see how synthetic biology is disrupting medicine. Register for SynBioBeta 2019: The Global Synthetic Biology Summit.

















